Payors & Providers: The Tech Closing the Gap
Healthcare has a long history of payors and providers operating in tension. One side manages costs and coverage; the other focuses on delivering care. Their incentives don’t always line up, their data rarely flows freely between them, and their technology systems are often built with no consideration for the other side’s needs. The result is a fragmented experience — for patients, for clinicians, and for the organizations trying to improve outcomes while keeping costs in check.
What’s changing that equation right now is purpose-built technology — platforms designed specifically for how payors manage populations and how providers make clinical decisions. These aren’t generic healthcare IT tools repurposed for different audiences. They’re built from the ground up with each stakeholder’s real workflows, real data challenges, and real accountability structures in mind.
What Payors Actually Need From a Health Platform
Running a health plan means managing risk across thousands — sometimes millions — of members. Most of those members are healthy most of the time. A small percentage drive a disproportionate share of cost. Identifying who’s in that high-risk segment, understanding why, and doing something useful about it before claims pile up — that’s the core challenge of payor population health management.
A purpose-built Payor Population Health Platform tackles this by aggregating claims data, pharmacy records, lab results, social determinants, and care gaps into a unified member profile — then applying predictive analytics to surface who needs intervention and when. Instead of reactive case management triggered by a crisis admission, care teams can act on risk signals weeks or months earlier, when interventions are cheaper and more effective.
For health plan medical directors and care management leadership, a Payor Population Health Platform also becomes a quality reporting engine. Star ratings, HEDIS metrics, and value-based contract performance all depend on closing care gaps systematically and documenting outreach consistently. Without a platform built to support those workflows, teams end up stitching together reports from multiple systems — and inevitably missing members who should have been reached.
There’s also a member engagement dimension that’s often underestimated. The best payor platforms don’t just identify risk — they support outreach, track touchpoints, and measure whether interventions are actually moving the needle. A care manager should be able to see, in a single view, that a high-risk member was contacted, what was discussed, what the care plan includes, and whether the member followed through. That closed loop is what turns data into outcomes.
Providers Need More Than an EHR Can Offer
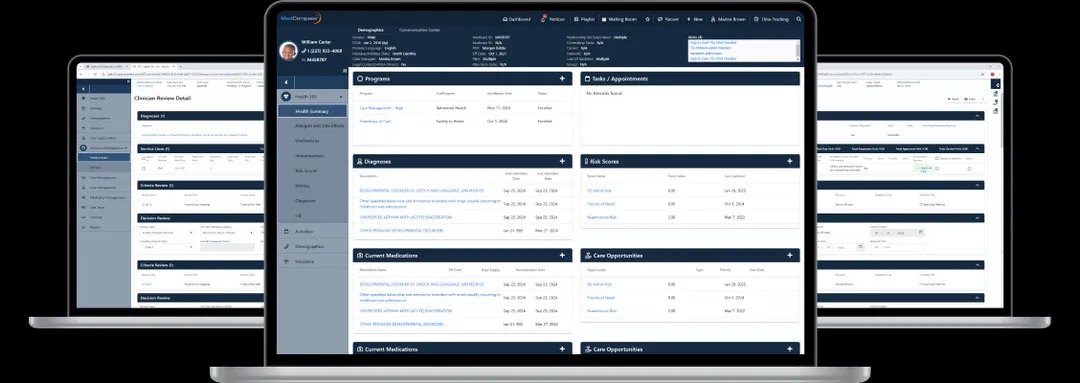
On the provider side, the challenge looks different but is equally real. Clinicians have access to more patient data than ever before — but more data doesn’t automatically mean better decisions. EHR systems were designed primarily for documentation and billing. They’re excellent at storing information; they’re not built to synthesize it, contextualize it across a population, or surface insights at the point of care in a way that’s actually actionable.
That’s the role a Clinical Insights Platform for Providers is built to fill. Rather than replacing the EHR, it works alongside it — pulling in data from multiple sources and translating it into clear, timely guidance that helps clinicians make better decisions without slowing down their workflow. Which patients on today’s schedule are overdue for a critical screening? Which recently discharged patients are at high risk for readmission in the next 30 days? Which chronic disease patients have had no engagement in six months? A Clinical Insights Platform for Providers answers those questions automatically, so care teams aren’t manually building queries or pulling reports between patient visits.
For provider organizations taking on value-based contracts, this capability is directly tied to financial performance. Under shared savings arrangements and risk-based models, providers are accountable for outcomes — not just encounters. Knowing which patients are falling through the cracks before the contract period ends is the difference between a shared savings payment and a shared loss conversation.
There’s a workforce dimension here too. Physicians and care teams are stretched thin. Administrative burden is one of the top drivers of clinical burnout. A well-designed clinical insights platform reduces that burden by doing the analytical heavy lifting — so that when a nurse practitioner walks into an exam room, they already know the three things that matter most for that patient, rather than spending the first five minutes of the visit figuring it out.
The Real Opportunity: Payor-Provider Alignment
The most forward-thinking organizations in healthcare right now are the ones figuring out how to make payor and provider data work together rather than in parallel. When a Payor Population Health Platform and a clinical insights platform share a common data foundation, both sides gain visibility they couldn’t have independently.
A health plan might know, through claims data, that a member hasn’t filled a critical maintenance medication in three months. The provider caring for that patient might not know, because the EHR only shows what happens inside their own walls. When those data streams connect, the provider gets an alert, the care manager knows to follow up, and the patient gets a phone call before they end up in the emergency department.
This kind of coordinated visibility isn’t theoretical — it’s the operational model that ACOs, integrated delivery networks, and progressive health plans are actively building toward. The technology has finally caught up to the concept.
Choosing the Right Platform for Your Organization
Whether you’re evaluating a Payor Population Health Platform or a clinical insights solution for your provider network, a few questions are worth asking before you commit:
Does it fit your existing workflows? The best platform in the world fails if your team works around it. Look for tools built with input from the actual users — care managers, UM nurses, clinicians — not just IT departments.
Can it connect with your existing data sources? Interoperability with your EHR, claims system, and HIE isn’t optional anymore. Siloed tools create more administrative work, not less.
Does it measure outcomes, not just activity? Tracking outreach calls is easy. Knowing whether those calls led to better adherence, fewer admissions, or improved quality scores is what actually matters.
Will it scale with you? Your member or patient population will grow and change. The platform should handle that without requiring a full reimplementation every few years.
Closing Thoughts
The divide between payors and providers has never been purely about incentives — it’s also been about information. Each side has data the other doesn’t, and the inability to act on a complete picture has cost the system enormously in unnecessary utilization, avoidable complications, and missed care opportunities.
Purpose-built platforms — a Payor Population Health Platform on one side, a Clinical Insights Platform for Providers on the other — are two pieces of the same solution. Together, they create the conditions for the kind of coordinated, data-informed care that healthcare has been working toward for decades. The technology is no longer the barrier. The question now is which organizations are ready to use it.
AssureCare builds solutions tailored for both payors and providers. Explore how at assurecare.com.
Share this content:








Post Comment